Pyoderma
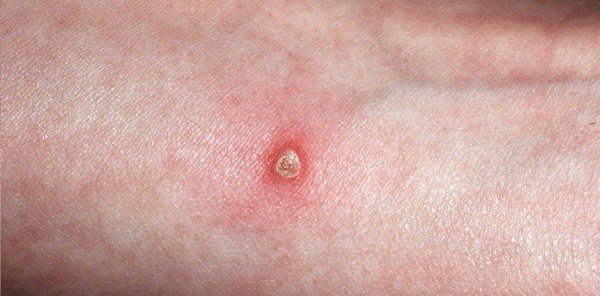
Pyoderma unites purulent-inflammatory skin diseases, the cause of which appears to be the microflora causing purulent infections – streptococci and staphylococci, commonly called pyococci.
Approximately 1/3 of all skin diseases represent various pyodermas.
Primary types of the disease occur when healthy skin is affected, and secondary types are a complication of other medical conditions in which skin damage due to scratching is possible.
As complications, pyoderma can develop with scabies, eczema, as well as with diabetes and chronic kidney failure.
In the complicated forms of the disease the damage to the skin is superficial and after healing the skin surface is completely restored.
But if the clinical condition assumes a chronic or excessively long course, it also affects the deeper layers of the skin and, accordingly, scars and dark spots remain.
What are the reasons?
On the surface of the human skin, a large amount of microorganisms constantly live, and some of them are part of the normal microflora of the skin.
Also, a part of these microorganisms are in a saprophytic or transitional form, and when the protective function of the skin decreases, it is possible for them to switch to an active form.
As a result of the vital activity of these microorganisms, enzymes, endo and exotoxins are released, which leads to a local skin reaction in the form of pyoderma.
In the pathogenesis of the disease, an important place is occupied by working conditions and the characteristics of the human skin, age and state of the immune system.
Decreasing the immunological reactivity of the person and failure to observe personal hygiene increase the probability of the occurrence of the clinical condition.
In most cases, the disease is the result of the saprophytic microflora, and for this reason the patients do not pose a danger to others.
Microtraumas, stressful situations, overheating or overcooling are factors that lead to a decrease in the skin’s protective function and, accordingly, increase the likelihood of developing the disease.
The risk group also includes people suffering from diabetes mellitus, pathologies of the digestive system, disorders in the hematopoietic process and vitamin balance, and obesity and chronic fatigue also contribute to the weakening of local immunity.
The skin is prone to the formation of large amounts of sebum in disorders of the central nervous system, which make the body susceptible to pyococci, because the change in the chemical composition of the sebum reduces the sterilization properties of the skin.
Changing hormonal levels or taking corticosteroids can lead to common diseases that appear to predispose to pyoderma.
Treatment of pyoderma
Treatment should be handled by a dermatologist.
When the focus of the infection is on the scalp, then the surrounding area is trimmed, but not shaved, to prevent the invasion of the pathogenic microflora in the healthy areas of the skin.
If the disease is of a generalized nature, water procedures are prohibited, including washing and washing. Contact with water is extremely undesirable, especially in the acute phase of the disease.
The skin around the affected area is treated with alcohol solutions of aniline derivatives and disinfectants. Salicylic acid and potassium permanganate solution also have a good effect.
Regardless of the fact that contact with water is prohibited, daily it is necessary to thoroughly wash hands and treat nails with 2% iodine solution to prevent infection, but healthy skin is also wiped with a previously disinfected wet sponge.< /p>
Food during treatment should be balanced, it is best to switch to a milk-vegetable diet. Alcohol should be completely excluded from the menu and the amount of salt and simple foods should be limited carbohydrates.



